|
In the case presented here, the subfoveal fluid was improving at the patient’s most recent visit, similar to what is seen in surgically closed MHs, but it may take a year or longer to fully resolve. In an analysis of OCT findings in surgically closed MHs in the PIONEER study, subfoveal fluid was present in 49% of eyes at 1 month after surgery, decreasing to 37% at 6 months. The hole closed, and likely over time the subfoveal fluid pocket will reabsorb. It stands to reason that, if the retinal hydration can be reduced medically, the MH should close without surgery, which it did in the case presented here. Surgery with internal limiting membrane peeling and gas bubble tamponade accomplishes this with a high degree of success. This theory suggests that reversing the hydration process may lead to hole closure.  
As the inner retina swells, it retracts anteriorly, widening the hole. In 2003, Tornambe proposed a hydration theory of MH formation, 1 whereby posterior hyaloid traction creates a small inner foveal retinal defect which then absorbs vitreous cavity fluid, causing retinal swelling around the defect. MHs are believed to form due to tractional forces at the vitreoretinal interface. At the patient’s last visit, at which point he was using ketorolac once daily, the MH remained closed with reduced subfoveal fluid and unchanged visual acuity or symptoms (Figure 4). Over the next 4 months, the drops were gradually tapered. 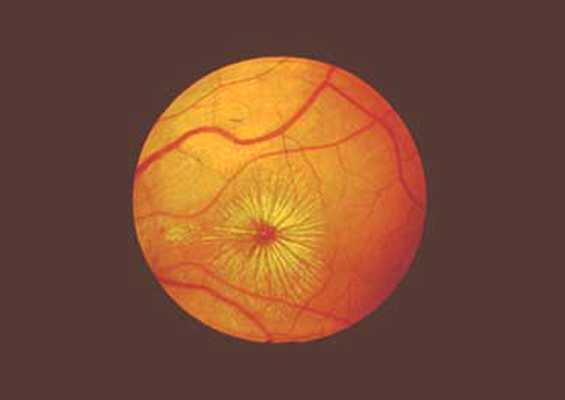
High-density OCT scan through the fovea 4 months after starting treatment showing a closed MH with a slightly smaller subfoveal fluid pocket.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
